Visceral Fat And Heart Health!
The Relationship Of Abdominal Fat And Heart Health!
When the Belly Shrinks, the Heart Sighs in Relief
There is a visible change when abdominal girth reduces. Clothes fit better. Movement feels lighter. Energy improves.
But there is also an invisible change — deeper, quieter, far more important.
The heart’s workload begins to fall.
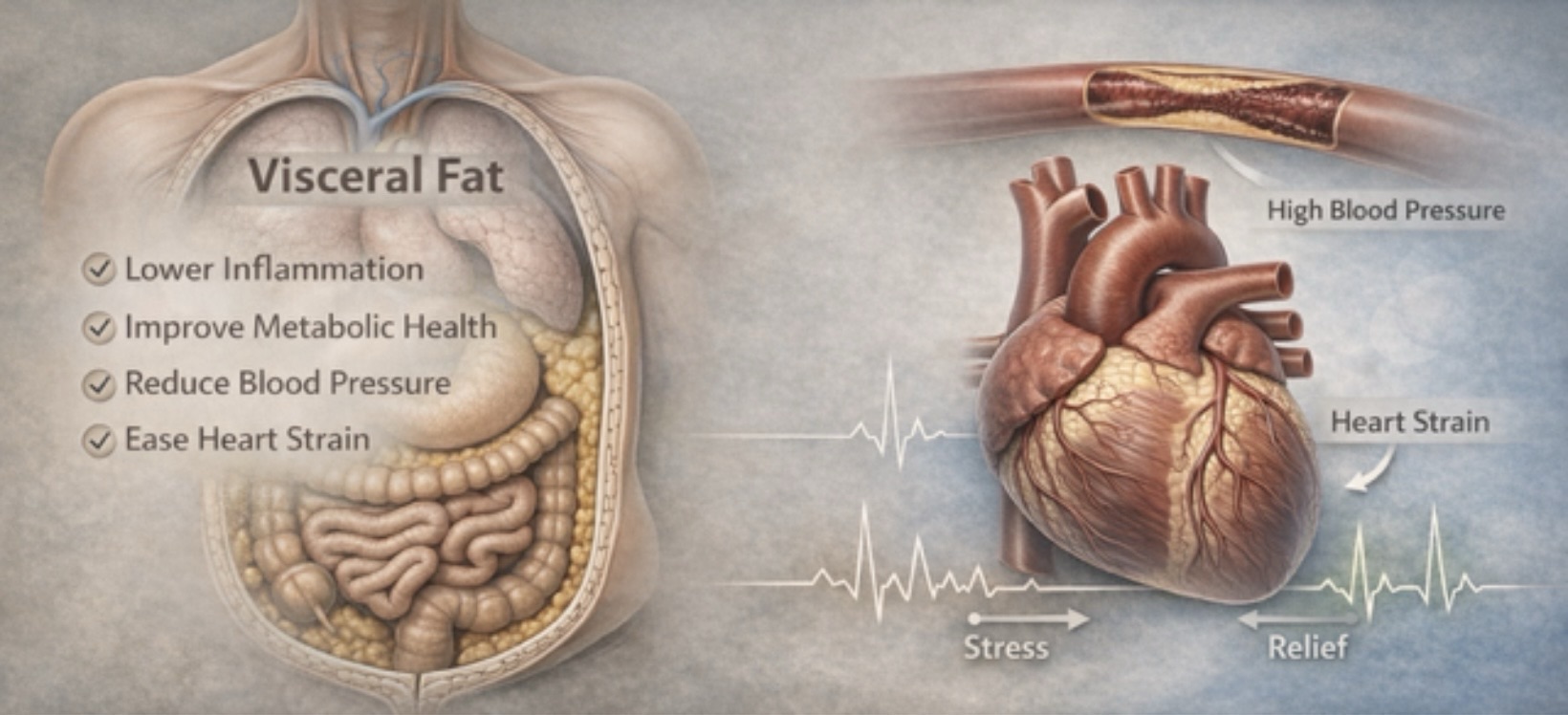
Visceral fat — the fat stored deep inside the abdomen around the liver, pancreas, and intestines — is not passive storage. It is biologically active tissue. It releases inflammatory chemicals, alters insulin sensitivity, increases blood pressure, and disrupts lipid metabolism.
It behaves less like stored fuel and more like an endocrine organ.
And the heart pays the price.
***
The Mechanical Burden
Every kilogram of excess tissue requires blood supply. More tissue means:
Greater total blood volume
Higher cardiac output
Increased pressure load
Thickening of the heart muscle over time
The heart must pump harder and more frequently to serve a larger metabolic territory.
When visceral fat reduces, circulating blood volume gradually decreases. Peripheral resistance improves. The demand on cardiac output falls. The heart can pump more efficiently, with less strain.
***
The Hormonal and Inflammatory Load
Visceral fat secretes pro-inflammatory cytokines and contributes to insulin resistance. This combination:
Stiffens arteries
Impairs endothelial function
Promotes plaque formation
Raises triglycerides
Lowers HDL cholesterol
Chronic low-grade inflammation keeps the vascular system in a constant state of irritation.
When visceral fat reduces, inflammatory markers like CRP often decline
Insulin sensitivity improves.
Blood pressure tends to fall
Lipid patterns shift favorably
The inner lining of the arteries — the endothelium — begins to function better.
Nitric oxide production improves
Arteries regain some of their flexibility.
And flexible arteries make the heart’s job easier.
***
The Blood Pressure Effect
Abdominal obesity is strongly linked with hypertension. Mechanisms include:
Activation of the sympathetic nervous system
Increased renin-angiotensin activity
Sodium retention
Arterial stiffness
Reduction in visceral fat often leads to measurable drops in systolic and diastolic blood pressure.
Even a 5–10% reduction in body weight can produce meaningful cardiovascular benefits.
Lower pressure means less resistance
Less resistance means less strain
Less strain means reduced risk of heart failure, stroke, and coronary events.
***
The Metabolic Reset
Visceral fat is central to metabolic syndrome — the cluster of:
Elevated fasting glucose
High triglycerides
Low HDL
Hypertension
Central obesity
As abdominal fat reduces, this cluster begins to unravel.
Insulin works better
The liver produces fewer atherogenic particles
Triglycerides fall
HDL may rise
Glycemic variability decreases
Each of these changes independently reduces cardiovascular risk. Together, they compound.
***
Structural Changes in the Heart
Over time, excess weight can cause:
Left ventricular hypertrophy
Diastolic dysfunction
Enlargement of cardiac chambers
Weight and visceral fat reduction have been shown to partially reverse some of these structural changes, especially when achieved early.
The heart remodels in a favorable direction.
It is not just about prevention. It is about recovery.
***
Beyond Numbers
The tape measure tells one story.
The scale tells another.
But the more meaningful shift happens at the cellular and vascular level.
When visceral fat decreases:
The inflammatory storm quiets
Arterial walls relax
Blood pressure softens
Glucose control stabilizes
The heart pumps against less resistance
The change is systemic
The abdomen becomes smaller
The arteries become healthier
The heart becomes less burdened
And the risk curve bends downward.
***
A Practical Perspective
This is not about cosmetic weight loss.
It is about reducing metabolic load.
Waist circumference is often a more useful marker of cardiovascular risk than weight alone.
A gradual, sustained reduction through:
Balanced nutrition
Regular aerobic activity
Resistance training
Adequate sleep
Stress reduction can produce profound internal change — even before dramatic visual transformation occurs.
A shrinking waist is not vanity.
It is vascular protection.
Related articles:
‘Abdominal Obesity, Diabetes and Heart Disease’
‘Waist Size, Blood Pressure, Blood Sugar And Heart Health!’.