Overcoming PCOS Or PMOS And Infertility: The Role Of Weight Loss in Fertility Treatment!
PCOS Or PMOS And Fertility: How Weight Loss Can Restore Ovulation!
The Critical Role of Weight Loss in PCOS Or PMOS!
***
PCOS Is Now Increasingly Being Called PMOS
An important recent development is that international experts have begun replacing the term PCOS with PMOS — Polyendocrine Metabolic Ovarian Syndrome.
The newer name reflects modern scientific understanding more accurately. Many women with the condition do not actually have ovarian cysts, while the disorder affects not only the ovaries, but also metabolism, insulin regulation, hormones, body fat distribution, emotional disturbances, skin, fertility and long-term cardiovascular health.
Many people are also familiar with the older term PCOD (Polycystic Ovarian Disease). Modern medical understanding now recognises that PCOD and PCOS largely refer to the same condition, with PCOS — and increasingly PMOS — being the preferred terminology.
Most importantly, PMOS is not merely an ovarian disorder. It is a complex condition involving the body’s metabolic and hormonal systems.
***
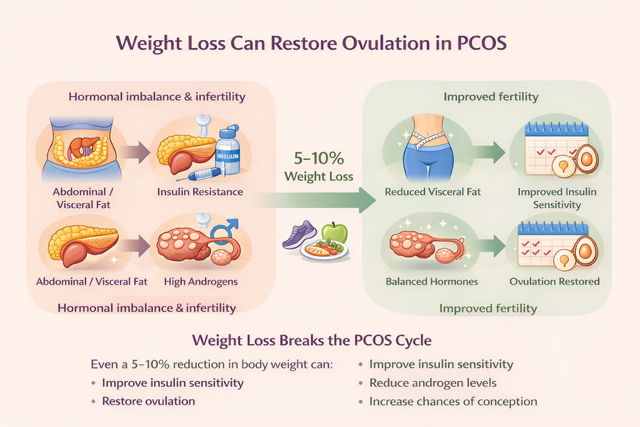
Many women with PMOS believe that infertility is caused mainly by ovarian cysts or hormonal imbalance. However, modern research shows that the real underlying driver in many cases is insulin resistance and excess abdominal fat. This metabolic disturbance interferes with ovulation and disrupts the delicate hormonal balance required for fertility. The encouraging news is that even modest weight loss – as little as 5 – 10% of body weight — can restore ovulation and significantly improve the chances of conception in many women with PMOS.
Key Points:
•PMOS is not only a reproductive disorder but also a metabolic condition linked to insulin resistance.
• Excess abdominal and visceral fat worsens hormonal imbalance and interferes with ovulation.
• Losing even 5–10% of body weight can restore ovulation in many women with PCOS.
• Weight loss improves insulin sensitivity, hormone balance and fertility outcomes.
• Lifestyle measures such as healthy diet, regular exercise and stress reduction form the foundation of treatment.
Introduction:
PMOS is one of the most common causes of infertility in women of reproductive age.
Women with PMOS may experience:
• Irregular or absent menstrual periods
• Difficulty conceiving
• Weight gain, especially around the abdomen
• Excess facial or body hair
• Acne or oily skin
• Emotional disturbances
While these symptoms are well recognised, PMOS is increasingly understood to be not only a reproductive disorder but also a metabolic condition closely linked to insulin resistance and abdominal fat accumulation.
Understanding this connection is essential for effective treatment.
The Metabolic Root of PMOS: Insulin Resistance:
Many women with PMOS have insulin resistance, a condition in which the body’s cells do not respond properly to insulin.
To compensate, the pancreas produces higher levels of insulin, a condition known as hyperinsulinaemia.
Elevated insulin levels contribute to several problems in PMOS:
• stimulation of the ovaries to produce excess male hormones (androgens)
• disruption of normal ovulation
• increased storage of fat, particularly in the abdominal region.
This leads to a vicious cycle:
Insulin resistance → High insulin levels → Increased androgens → Irregular ovulation → Weight gain → Worsening insulin resistance.
Breaking this cycle is key to restoring normal fertility.
The Role of Abdominal and Visceral Fat:
Women with PMOS often accumulate fat around the abdomen, particularly visceral fat.
Visceral fat is the fat stored deep inside the abdomen around internal organs. Unlike fat under the skin, it is metabolically active and releases substances that worsen:
• insulin resistance
• inflammation
• hormonal imbalance.
Even women who are not visibly obese may still have excess visceral fat and metabolic disturbances.
This is why reducing abdominal fat is often more important than simply reducing overall body weight.
Can Weight Loss Help PMOS?
Yes. Weight loss plays a crucial role in improving the hormonal and metabolic disturbances associated with PMOS.
Excess body fat, especially abdominal fat, worsens insulin resistance and leads to higher insulin levels. This in turn stimulates the ovaries to produce excess male hormones, which interfere with ovulation.
Reducing body weight helps to:
• improve insulin sensitivity
• lower insulin levels
• reduce androgen production
• restore more regular ovulation.
Even modest weight reduction can therefore break the metabolic cycle that contributes to PMOS symptoms and infertility.
How Weight Loss Improves Fertility:
The encouraging news is that even modest weight loss can significantly improve reproductive function in women with PMOS.
Studies have shown that losing just 5–10% of body weight can:
• improve insulin sensitivity
• reduce androgen levels
• restore ovulation
• regulate menstrual cycles
• increase the chances of natural conception.
In some women, ovulation resumes naturally once metabolic health improves.
Weight loss also improves the success rates of fertility treatments when they are required.
Lifestyle Treatment Should Be the First Step:
In many cases, lifestyle modification should be the first line of treatment before medications or assisted reproductive techniques.
A well-designed program should focus on three key pillars.
1. Dietary Changes
The goal of dietary treatment is to reduce insulin levels and promote gradual fat loss.
Helpful strategies include:
• reducing refined carbohydrates and sugars
• increasing protein intake
• consuming more fibre-rich foods such as vegetables and whole grains
• including healthy fats
• controlling portion sizes.
These changes help stabilise blood sugar and reduce insulin spikes.
2. Regular Physical Activity
Exercise improves insulin sensitivity and helps reduce abdominal fat.
A balanced routine may include:
• brisk walking or jogging
• strength training or resistance exercises
• yoga or relaxation techniques.
Regular physical activity also improves mood and reduces stress.
3. Stress Reduction and Adequate Sleep:
Chronic stress and poor sleep can worsen hormonal imbalance and insulin resistance.
Relaxation techniques such as meditation, yoga, or guided relaxation may help restore metabolic balance.
The Benefits Extend Beyond Fertility:
Addressing the metabolic aspects of PMOS does more than improve fertility.
It also reduces the long-term risk of:
• type 2 diabetes
• high blood pressure
• heart disease
• metabolic syndrome.
Thus, lifestyle treatment benefits both reproductive health and long-term health.
A Message of Hope:
PMOS can be frustrating and emotionally distressing, especially for women trying to conceive.
However, the condition is highly responsive to lifestyle changes.
With sustained weight management, improved diet and regular exercise, many women can restore ovulation and significantly improve their chances of conception.
In many cases, correcting the underlying metabolic imbalance becomes the most effective step toward overcoming PMOS-related infertility.
Doctor’s Insight
PMOS Is Often a Metabolic Disorder First
Many women think of PMOS only as a hormonal disorder affecting the ovaries. In reality, insulin resistance and abdominal fat accumulation are often the underlying drivers. Treating these metabolic factors frequently improves both hormonal balance and fertility.
Even Small Weight Loss Can Make a Big Difference:
Patients are often surprised to learn that a modest reduction in body weight can restore ovulation. The goal is not extreme dieting but sustainable lifestyle changes that reduce visceral fat and improve metabolic health.
Frequently Asked Questions:
Can weight loss really improve fertility in women with PMOS?
Yes. Even a modest weight loss of 5–10% of body weight can significantly improve fertility in many women with PMOS. Weight loss improves insulin sensitivity, reduces excess male hormones (androgens), and helps restore regular ovulation.
Is PMOS mainly a hormonal disorder or a metabolic disorder?
PMOS is both a hormonal and metabolic condition. While hormonal imbalance affects ovulation and menstrual cycles, insulin resistance and abdominal fat accumulation are major underlying factors in many women with PMOS.
Can women with PMOS conceive naturally?
Yes. Many women with PMOS are able to conceive naturally, especially after improving metabolic health through weight reduction, healthy diet and regular exercise.
Article Update:
This article was reviewed and updated to reflect current understanding of the metabolic aspects of PMOS, including the role of insulin resistance and abdominal fat in infertility.
***
Related articles:













Leave a Reply