Posts Shortcodes
You can show the posts with Porto Blog, Porto Recent Posts shortcodes.
Recent
Timeline
May 2026
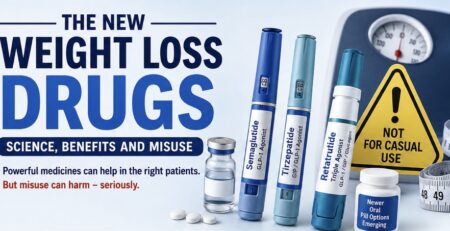
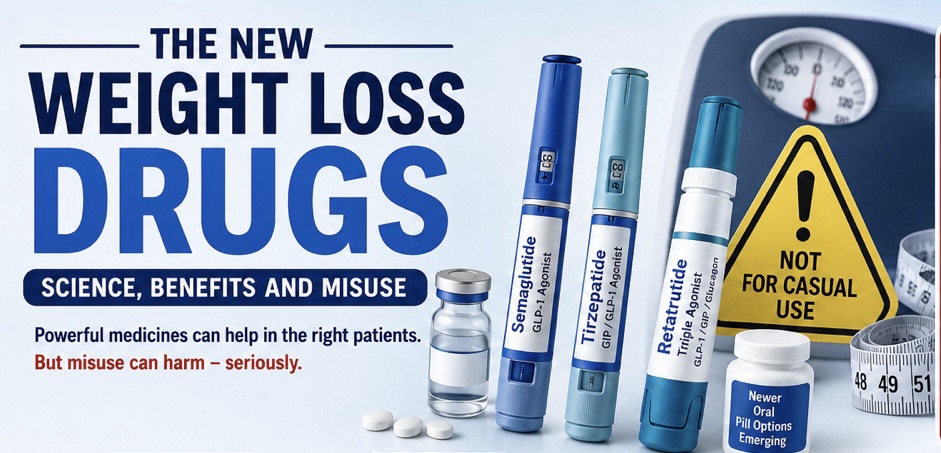
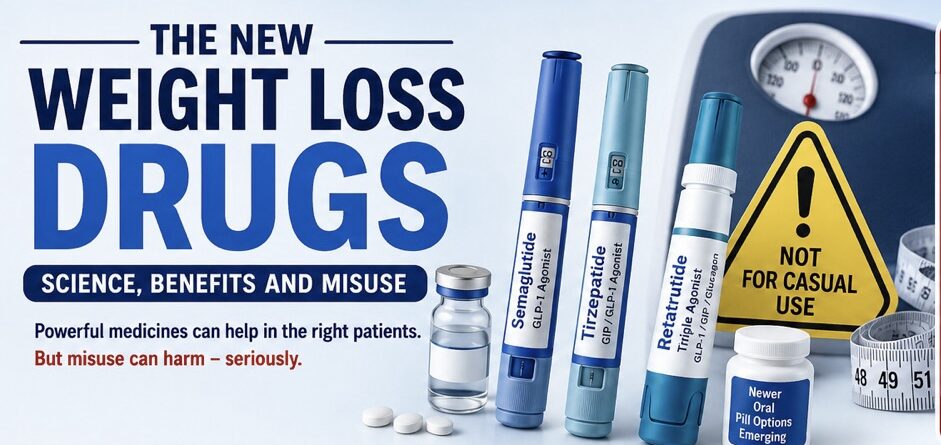
The New Weight Loss Drugs — Science, Benefits And Misuse!
Benefits As Medical Treatment And Dangers Of Unethical, Casual Use!
A new class of medicines originally developed for diabetes has rapidly become the centre of a global weight loss craze.
Celebrities, influencers and social media personalities are discussing these injections as if they are shortcuts to an ideal body. Increasingly, even people who need to lose only a few kilograms are asking doctors whether they should start these medicines.
This trend needs careful scientific understanding.
***
What Are These Medicines?
The most commonly discussed drugs belong to a group called GLP-1 receptor agonists and related medicines.
Examples include:
Semaglutide
Tirzepatide
Liraglutide
Researchers are also developing newer and more powerful medicines including dual-agonist and triple-agonist drugs that act on multiple hormonal pathways related to appetite, metabolism and blood sugar control.
Some of the newer medicines attracting attention include:
Retatrutide
Orforglipron
CagriSema
Oral pill versions of some of these medicines are also becoming available, which may further increase their popularity and commercial use in the coming years.
While these newer drugs may improve weight loss in selected patients, they also raise concerns about increasing casual use, aggressive marketing and long-term overmedicalisation of body weight.
These medicines were originally developed for treating type 2 diabetes. Doctors later observed that many patients also lost weight while taking them.
***
How Do They Work?
These drugs mainly:
reduce appetite,
increase the feeling of fullness,
slow stomach emptying,
and improve blood sugar control.
Many patients naturally eat less while taking them.
***
Can They Help?
Yes — in properly selected overweight or obese individuals, especially those with:
diabetes,
prediabetes,
fatty liver disease,
metabolic syndrome,
abdominal obesity,
hypertension,
or sleep apnoea,
these medicines can sometimes produce meaningful weight reduction and metabolic improvement.
For severely obese individuals struggling despite sincere lifestyle changes, they may reduce long-term health risks.
***
The Growing Misuse
The problem is that these medicines are increasingly being used by:
mildly overweight people,
individuals wanting “camera-ready” appearances,
young adults influenced by social media,
and even normal-weight individuals afraid of gaining weight.
Medicines meant for obesity and metabolic disease are slowly being turned into cosmetic lifestyle products.
Weight Loss Alone Is Not Health
A person may lose weight and still become unhealthy.
Rapid weight loss without proper nutrition may reduce:
muscle mass,
strength,
stamina,
and nutritional reserves.
Especially in middle-aged and older individuals, excessive muscle loss can become a serious long-term problem.
The goal should not merely be ‘lighter weight’, but:
healthier metabolism,
lower abdominal fat,
improved strength,
better fitness,
and sustainable habits.
***
These Medicines Require Specialist Supervision
These are powerful prescription medicines and are usually best supervised by endocrinologists, diabetologists or cardiologists familiar with obesity-related metabolic disease.
Before starting treatment, doctors may need to assess:
blood sugar,
kidney and liver function,
pancreatic and gall bladder health,
cardiovascular risk,
nutritional status,
and existing medications.
Careful follow-up is important to monitor:
side effects,
hydration,
nutritional adequacy,
and muscle preservation.
***
Using these medicines casually for cosmetic slimming without proper supervision may expose otherwise healthy individuals to unnecessary risks.
Possible Side Effects
Common side effects include:
nausea,
vomiting,
acidity,
constipation,
diarrhoea,
bloating,
and fatigue.
More serious concerns may include:
gall bladder disease,
pancreatitis,
dehydration,
nutritional deficiencies,
and excessive muscle loss.
***
Another Important Reality — Weight Often Returns
Many people regain weight after stopping the medicine if lifestyle habits have not changed.
These medicines cannot permanently replace:
dietary discipline,
physical activity,
sleep regulation,
and behavioural change.
***
Final Message
These newer medicines represent an important scientific advance in obesity treatment and may genuinely help selected patients.
But their growing misuse reflects a larger commercial culture obsessed with appearance and rapid slimming.
Most of the use of these powerful prescription drugs in India is unethical, likely suggested by gym trainers and beauty clinics and word of mouth in social circles and parties, often procured from grey markets.
Such use is extremely dangerous.
Health should remain the primary goal — not simply becoming thinner for photographs, social approval or social media trends.
Related article
April 2026
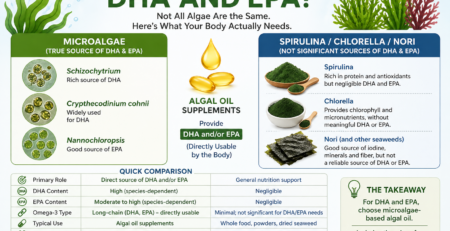
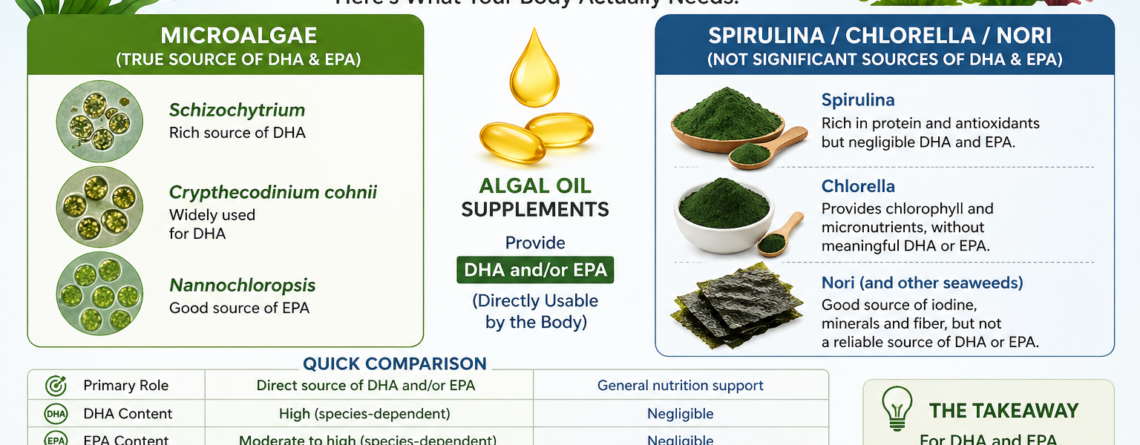
Which Algae Provide DHA And EPA?
Microalgae, Spirulina, Chlorella And Nori!
Why Most ‘Algae Superfoods” Don’t Meet Your Omega-3 Needs?
Most algae are promoted as nutritional superfoods—but not all of them provide the omega-3 fats your body actually needs. If you are relying on spirulina, chlorella, or seaweed for DHA and EPA, you may be missing a critical piece of the puzzle. This article explains which algae truly deliver these essential fats—and which do not.
Microalgae: The True Source Of DHA And EPA
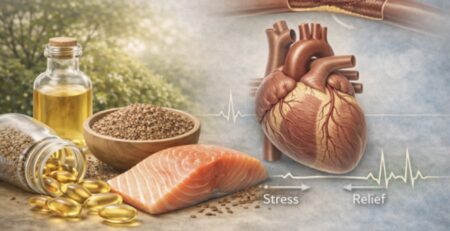
DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) originate in marine microalgae—not in fish. Fish accumulate these fats by consuming algae, making microalgae the primary source in the food chain.
Certain species of microalgae are particularly rich in these long-chain omega-3s, DHA and EPA:
Schizochytrium – a concentrated source of DHA
Crypthecodinium cohnii – widely used for its DHA content
Nannochloropsis – a valuable source of EPA
These microalgae are cultivated and processed into algal oil, which forms the basis of most vegetarian and vegan omega-3 supplements. Unlike plant sources such as flaxseeds or walnuts, which provide ALA (alpha-linolenic acid), these deliver DHA and EPA directly—the forms the body actually uses.
This distinction matters because the conversion of ALA to DHA and EPA in humans is inefficient and often insufficient to meet physiological needs.
***
What Can You Actually Buy?
In practical terms, microalgae are not consumed directly as foods—they are available as algal oil supplements.
These typically come in:
Softgel capsules (most common)
Liquid algal oil (less common)
Most products provide DHA alone or a combination of DHA and EPA, usually in the range of 100–300 mg per serving. They are plant-based, fish-free, and sourced from controlled cultivation, making them a clean alternative to fish oil.
When choosing a supplement, the most useful label to check is the actual DHA and EPA content per serving, rather than just the term ‘omega-3’.
Other Algae: Nutritious, But Not Omega-3 Sources
Commonly consumed algae contribute valuable nutrients, but not meaningful amounts of DHA or EPA:
Spirulina – rich in protein and antioxidants like phycocyanin, but contains negligible DHA and EPA.
Chlorella – provides chlorophyll and micronutrients, without contributing significant DHA and EPA.
Nori (and other seaweeds) – a useful source of iodine, trace minerals, and fiber, but not a reliable source of DHA or EPA.
***
Why This Matters
Confusing these categories can create a false sense of nutritional adequacy. Regular intake of spirulina or seaweed does not ensure sufficient DHA and EPA.
For those who do not consume fatty fish, this gap is important, as DHA and EPA play key roles in brain function, vision, inflammation regulation, and cardiovascular health.
***
Quick Comparison: Microalgae Vs Common Edible Algae
Omega-3 From Algae: What Actually Works?
Microalgae: The Real Omega-3 Sources
Provides DHA and EPA (directly usable forms)
Examples: Schizochytrium, Nannochloropsis
Used as algal oil supplements
Supports: Brain • Eyes • Heart • Anti-inflammatory
Common Edible Algae Or Seaweed: Spirulina / Chlorella / Nori: The Non Omega-3 Nutritional Supplements:
Negligible DHA and EPA
Provide: Protein • Minerals • Antioxidants • Iodine
Useful for general nutrition, but not for omega-3 needs
***
Practical Takeaway
Use microalgae-derived algal oil to obtain DHA and EPA
Include other algae for their general nutritional value, not for omega-3s
Do not rely solely on ALA sources for providing long-chain omega-3, DHA and EPA
***
Conclusion
Algae are very good sources of nutrition, but not all of them provide DHA and EPA. Microalgae-derived algal oil provides a direct, effective source of DHA and EPA, while other algae serve as supportive, nutrient-rich foods.
Related articles:
Grid
The New Weight Loss Drugs — Science, Benefits And Misuse!
Benefits As Medical Treatment And Dangers Of Unethical, Casual Use!
A new class of medicines originally developed for diabetes has rapidly become the centre of a global weight loss craze.
Celebrities, influencers and social media personalities are discussing these injections as if they are shortcuts to an ideal body. Increasingly, even people who need to lose only a few kilograms are asking doctors whether they should start these medicines.
This trend needs careful scientific understanding.
***
What Are These Medicines?
The most commonly discussed drugs belong to a group called GLP-1 receptor agonists and related medicines.
Examples include:
Semaglutide
Tirzepatide
Liraglutide
Researchers are also developing newer and more powerful medicines including dual-agonist and triple-agonist drugs that act on multiple hormonal pathways related to appetite, metabolism and blood sugar control.
Some of the newer medicines attracting attention include:
Retatrutide
Orforglipron
CagriSema
Oral pill versions of some of these medicines are also becoming available, which may further increase their popularity and commercial use in the coming years.
While these newer drugs may improve weight loss in selected patients, they also raise concerns about increasing casual use, aggressive marketing and long-term overmedicalisation of body weight.
These medicines were originally developed for treating type 2 diabetes. Doctors later observed that many patients also lost weight while taking them.
***
How Do They Work?
These drugs mainly:
reduce appetite,
increase the feeling of fullness,
slow stomach emptying,
and improve blood sugar control.
Many patients naturally eat less while taking them.
***
Can They Help?
Yes — in properly selected overweight or obese individuals, especially those with:
diabetes,
prediabetes,
fatty liver disease,
metabolic syndrome,
abdominal obesity,
hypertension,
or sleep apnoea,
these medicines can sometimes produce meaningful weight reduction and metabolic improvement.
For severely obese individuals struggling despite sincere lifestyle changes, they may reduce long-term health risks.
***
The Growing Misuse
The problem is that these medicines are increasingly being used by:
mildly overweight people,
individuals wanting “camera-ready” appearances,
young adults influenced by social media,
and even normal-weight individuals afraid of gaining weight.
Medicines meant for obesity and metabolic disease are slowly being turned into cosmetic lifestyle products.
Weight Loss Alone Is Not Health
A person may lose weight and still become unhealthy.
Rapid weight loss without proper nutrition may reduce:
muscle mass,
strength,
stamina,
and nutritional reserves.
Especially in middle-aged and older individuals, excessive muscle loss can become a serious long-term problem.
The goal should not merely be ‘lighter weight’, but:
healthier metabolism,
lower abdominal fat,
improved strength,
better fitness,
and sustainable habits.
***
These Medicines Require Specialist Supervision
These are powerful prescription medicines and are usually best supervised by endocrinologists, diabetologists or cardiologists familiar with obesity-related metabolic disease.
Before starting treatment, doctors may need to assess:
blood sugar,
kidney and liver function,
pancreatic and gall bladder health,
cardiovascular risk,
nutritional status,
and existing medications.
Careful follow-up is important to monitor:
side effects,
hydration,
nutritional adequacy,
and muscle preservation.
***
Using these medicines casually for cosmetic slimming without proper supervision may expose otherwise healthy individuals to unnecessary risks.
Possible Side Effects
Common side effects include:
nausea,
vomiting,
acidity,
constipation,
diarrhoea,
bloating,
and fatigue.
More serious concerns may include:
gall bladder disease,
pancreatitis,
dehydration,
nutritional deficiencies,
and excessive muscle loss.
***
Another Important Reality — Weight Often Returns
Many people regain weight after stopping the medicine if lifestyle habits have not changed.
These medicines cannot permanently replace:
dietary discipline,
physical activity,
sleep regulation,
and behavioural change.
***
Final Message
These newer medicines represent an important scientific advance in obesity treatment and may genuinely help selected patients.
But their growing misuse reflects a larger commercial culture obsessed with appearance and rapid slimming.
Most of the use of these powerful prescription drugs in India is unethical, likely suggested by gym trainers and beauty clinics and word of mouth in social circles and parties, often procured from grey markets.
Such use is extremely dangerous.
Health should remain the primary goal — not simply becoming thinner for photographs, social approval or social media trends.
Related article
Which Algae Provide DHA And EPA?
Microalgae, Spirulina, Chlorella And Nori!
Why Most ‘Algae Superfoods” Don’t Meet Your Omega-3 Needs?
Most algae are promoted as nutritional superfoods—but not all of them provide the omega-3 fats your body actually needs. If you are relying on spirulina, chlorella, or seaweed for DHA and EPA, you may be missing a critical piece of the puzzle. This article explains which algae truly deliver these essential fats—and which do not.
Microalgae: The True Source Of DHA And EPA
DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) originate in marine microalgae—not in fish. Fish accumulate these fats by consuming algae, making microalgae the primary source in the food chain.
Certain species of microalgae are particularly rich in these long-chain omega-3s, DHA and EPA:
Schizochytrium – a concentrated source of DHA
Crypthecodinium cohnii – widely used for its DHA content
Nannochloropsis – a valuable source of EPA
These microalgae are cultivated and processed into algal oil, which forms the basis of most vegetarian and vegan omega-3 supplements. Unlike plant sources such as flaxseeds or walnuts, which provide ALA (alpha-linolenic acid), these deliver DHA and EPA directly—the forms the body actually uses.
This distinction matters because the conversion of ALA to DHA and EPA in humans is inefficient and often insufficient to meet physiological needs.
***
What Can You Actually Buy?
In practical terms, microalgae are not consumed directly as foods—they are available as algal oil supplements.
These typically come in:
Softgel capsules (most common)
Liquid algal oil (less common)
Most products provide DHA alone or a combination of DHA and EPA, usually in the range of 100–300 mg per serving. They are plant-based, fish-free, and sourced from controlled cultivation, making them a clean alternative to fish oil.
When choosing a supplement, the most useful label to check is the actual DHA and EPA content per serving, rather than just the term ‘omega-3’.
Other Algae: Nutritious, But Not Omega-3 Sources
Commonly consumed algae contribute valuable nutrients, but not meaningful amounts of DHA or EPA:
Spirulina – rich in protein and antioxidants like phycocyanin, but contains negligible DHA and EPA.
Chlorella – provides chlorophyll and micronutrients, without contributing significant DHA and EPA.
Nori (and other seaweeds) – a useful source of iodine, trace minerals, and fiber, but not a reliable source of DHA or EPA.
***
Why This Matters
Confusing these categories can create a false sense of nutritional adequacy. Regular intake of spirulina or seaweed does not ensure sufficient DHA and EPA.
For those who do not consume fatty fish, this gap is important, as DHA and EPA play key roles in brain function, vision, inflammation regulation, and cardiovascular health.
***
Quick Comparison: Microalgae Vs Common Edible Algae
Omega-3 From Algae: What Actually Works?
Microalgae: The Real Omega-3 Sources
Provides DHA and EPA (directly usable forms)
Examples: Schizochytrium, Nannochloropsis
Used as algal oil supplements
Supports: Brain • Eyes • Heart • Anti-inflammatory
Common Edible Algae Or Seaweed: Spirulina / Chlorella / Nori: The Non Omega-3 Nutritional Supplements:
Negligible DHA and EPA
Provide: Protein • Minerals • Antioxidants • Iodine
Useful for general nutrition, but not for omega-3 needs
***
Practical Takeaway
Use microalgae-derived algal oil to obtain DHA and EPA
Include other algae for their general nutritional value, not for omega-3s
Do not rely solely on ALA sources for providing long-chain omega-3, DHA and EPA
***
Conclusion
Algae are very good sources of nutrition, but not all of them provide DHA and EPA. Microalgae-derived algal oil provides a direct, effective source of DHA and EPA, while other algae serve as supportive, nutrient-rich foods.
Related articles:
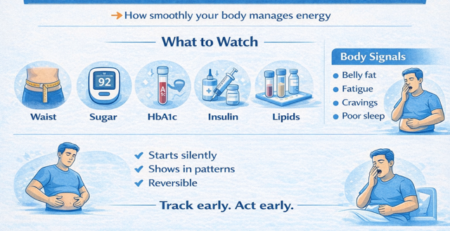
Metabolic Health — The Real Foundation of Well-Being!
Assessing Our Metabolic Health!
What is metabolic health?
Metabolic health is how efficiently your body:
- Uses and stores energy
- Maintains stable blood sugar
- Regulates insulin, blood pressure, and lipids
In simple terms:
It’s how smoothly your body runs its ‘energy system.’
***
You can feel ‘normal’ and still have underlying metabolic strain—because early changes are often silent.
Why It Matters
Good metabolic health supports:
- Steady energy
- Clear thinking
- Healthy weight regulation
- Heart health
- Hormonal balance
Poor metabolic health, over time, can lead to:
- Pre diabetes and diabetes
- Fatty liver
- Heart disease
- Chronic fatigue
***
How to Assess Your Metabolic Fitness
Instead of relying on just one number, look at a pattern of markers.
1. Abdominal Circumference: Your First Clue
- Men: ideally < 90 cm (35 inches)
- Women: ideally < 80 cm (31 inches)
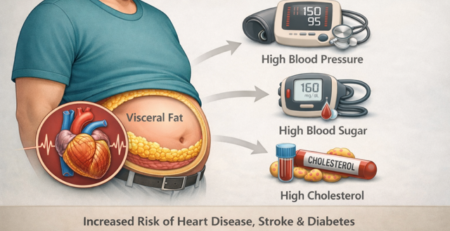
Increasing waist size is the early sign of visceral fat and metabolic stress
2. Fasting Blood Sugar
- Ideal: < 85–90 mg/dL
Even “normal” high values may indicate early imbalance
3. HbA1c: 3 Month Sugar Trend
- Ideal: ≤ 5.3–5.5%
- Rising trend = warning sign
Reflects long-term sugar exposure, not just one reading
4. Fasting Insulin: The Hidden Marker
- Ideal: < 6–8
- Concern: > 8–10
High insulin means your body and pancreas are over straining to keep blood sugars normal
5. Lipid Pattern: Don’t Watch Just Total Cholesterol
Also watch for:
- Raised Triglycerides
- Lowered HDL
- TG/HDL ratio > 2
This pattern suggests insulin resistance
6. Blood Pressure
- Ideal: Between 110–120 / 70–80
Even mildly elevated levels can reflect metabolic strain
7. Everyday Body Signals (Often Ignored)
***
Your body gives early clues:
- Increasing belly fat
- Fatigue or low energy
- Sugar cravings
- Poor sleep
- Darkening of neck skin
These are not minor symptoms —they’re early metabolic warnings
***
The Key Insight
Metabolic dysfunction develops gradually.
It starts before disease
It shows up in patterns—not isolated reports
It is reversible with the right lifestyle changes
***
Takeaway:
Don’t wait for a diagnosis.
Track these markers early, watch trends, and listen to your body.
Good metabolic health isn’t accidental—it’s built daily.
Related articles:
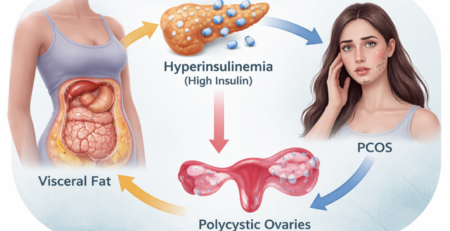
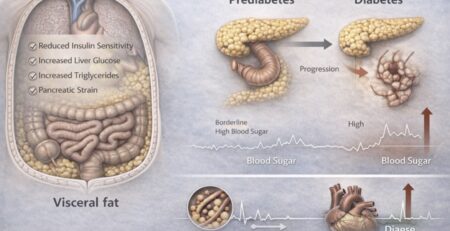
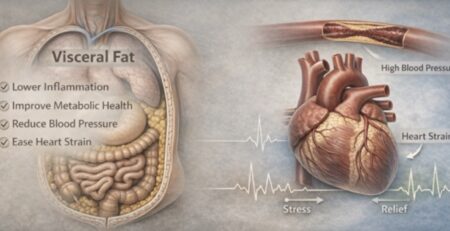
‘Interrelationship Between Visceral Fat, Inflammation And Metabolic Syndrome!’
Medium
The New Weight Loss Drugs — Science, Benefits And Misuse!
Benefits As Medical Treatment And Dangers Of Unethical, Casual Use!
A new class of medicines originally developed for diabetes has rapidly become the centre of a global weight loss craze.
Celebrities, influencers and social media personalities are discussing these injections as if they are shortcuts to an ideal body. Increasingly, even people who need to lose only a few kilograms are asking doctors whether they should start these medicines.
This trend needs careful scientific understanding.
***
What Are These Medicines?
The most commonly discussed drugs belong to a group called GLP-1 receptor agonists and related medicines.
Examples include:
Semaglutide
Tirzepatide
Liraglutide
Researchers are also developing newer and more powerful medicines including dual-agonist and triple-agonist drugs that act on multiple hormonal pathways related to appetite, metabolism and blood sugar control.
Some of the newer medicines attracting attention include:
Retatrutide
Orforglipron
CagriSema
Oral pill versions of some of these medicines are also becoming available, which may further increase their popularity and commercial use in the coming years.
While these newer drugs may improve weight loss in selected patients, they also raise concerns about increasing casual use, aggressive marketing and long-term overmedicalisation of body weight.
These medicines were originally developed for treating type 2 diabetes. Doctors later observed that many patients also lost weight while taking them.
***
How Do They Work?
These drugs mainly:
reduce appetite,
increase the feeling of fullness,
slow stomach emptying,
and improve blood sugar control.
Many patients naturally eat less while taking them.
***
Can They Help?
Yes — in properly selected overweight or obese individuals, especially those with:
diabetes,
prediabetes,
fatty liver disease,
metabolic syndrome,
abdominal obesity,
hypertension,
or sleep apnoea,
these medicines can sometimes produce meaningful weight reduction and metabolic improvement.
For severely obese individuals struggling despite sincere lifestyle changes, they may reduce long-term health risks.
***
The Growing Misuse
The problem is that these medicines are increasingly being used by:
mildly overweight people,
individuals wanting “camera-ready” appearances,
young adults influenced by social media,
and even normal-weight individuals afraid of gaining weight.
Medicines meant for obesity and metabolic disease are slowly being turned into cosmetic lifestyle products.
Weight Loss Alone Is Not Health
A person may lose weight and still become unhealthy.
Rapid weight loss without proper nutrition may reduce:
muscle mass,
strength,
stamina,
and nutritional reserves.
Especially in middle-aged and older individuals, excessive muscle loss can become a serious long-term problem.
The goal should not merely be ‘lighter weight’, but:
healthier metabolism,
lower abdominal fat,
improved strength,
better fitness,
and sustainable habits.
***
These Medicines Require Specialist Supervision
These are powerful prescription medicines and are usually best supervised by endocrinologists, diabetologists or cardiologists familiar with obesity-related metabolic disease.
Before starting treatment, doctors may need to assess:
blood sugar,
kidney and liver function,
pancreatic and gall bladder health,
cardiovascular risk,
nutritional status,
and existing medications.
Careful follow-up is important to monitor:
side effects,
hydration,
nutritional adequacy,
and muscle preservation.
***
Using these medicines casually for cosmetic slimming without proper supervision may expose otherwise healthy individuals to unnecessary risks.
Possible Side Effects
Common side effects include:
nausea,
vomiting,
acidity,
constipation,
diarrhoea,
bloating,
and fatigue.
More serious concerns may include:
gall bladder disease,
pancreatitis,
dehydration,
nutritional deficiencies,
and excessive muscle loss.
***
Another Important Reality — Weight Often Returns
Many people regain weight after stopping the medicine if lifestyle habits have not changed.
These medicines cannot permanently replace:
dietary discipline,
physical activity,
sleep regulation,
and behavioural change.
***
Final Message
These newer medicines represent an important scientific advance in obesity treatment and may genuinely help selected patients.
But their growing misuse reflects a larger commercial culture obsessed with appearance and rapid slimming.
Most of the use of these powerful prescription drugs in India is unethical, likely suggested by gym trainers and beauty clinics and word of mouth in social circles and parties, often procured from grey markets.
Such use is extremely dangerous.
Health should remain the primary goal — not simply becoming thinner for photographs, social approval or social media trends.
Related article
Which Algae Provide DHA And EPA?
Microalgae, Spirulina, Chlorella And Nori!
Why Most ‘Algae Superfoods” Don’t Meet Your Omega-3 Needs?
Most algae are promoted as nutritional superfoods—but not all of them provide the omega-3 fats your body actually needs. If you are relying on spirulina, chlorella, or seaweed for DHA and EPA, you may be missing a critical piece of the puzzle. This article explains which algae truly deliver these essential fats—and which do not.
Microalgae: The True Source Of DHA And EPA
DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) originate in marine microalgae—not in fish. Fish accumulate these fats by consuming algae, making microalgae the primary source in the food chain.
Certain species of microalgae are particularly rich in these long-chain omega-3s, DHA and EPA:
Schizochytrium – a concentrated source of DHA
Crypthecodinium cohnii – widely used for its DHA content
Nannochloropsis – a valuable source of EPA
These microalgae are cultivated and processed into algal oil, which forms the basis of most vegetarian and vegan omega-3 supplements. Unlike plant sources such as flaxseeds or walnuts, which provide ALA (alpha-linolenic acid), these deliver DHA and EPA directly—the forms the body actually uses.
This distinction matters because the conversion of ALA to DHA and EPA in humans is inefficient and often insufficient to meet physiological needs.
***
What Can You Actually Buy?
In practical terms, microalgae are not consumed directly as foods—they are available as algal oil supplements.
These typically come in:
Softgel capsules (most common)
Liquid algal oil (less common)
Most products provide DHA alone or a combination of DHA and EPA, usually in the range of 100–300 mg per serving. They are plant-based, fish-free, and sourced from controlled cultivation, making them a clean alternative to fish oil.
When choosing a supplement, the most useful label to check is the actual DHA and EPA content per serving, rather than just the term ‘omega-3’.
Other Algae: Nutritious, But Not Omega-3 Sources
Commonly consumed algae contribute valuable nutrients, but not meaningful amounts of DHA or EPA:
Spirulina – rich in protein and antioxidants like phycocyanin, but contains negligible DHA and EPA.
Chlorella – provides chlorophyll and micronutrients, without contributing significant DHA and EPA.
Nori (and other seaweeds) – a useful source of iodine, trace minerals, and fiber, but not a reliable source of DHA or EPA.
***
Why This Matters
Confusing these categories can create a false sense of nutritional adequacy. Regular intake of spirulina or seaweed does not ensure sufficient DHA and EPA.
For those who do not consume fatty fish, this gap is important, as DHA and EPA play key roles in brain function, vision, inflammation regulation, and cardiovascular health.
***
Quick Comparison: Microalgae Vs Common Edible Algae
Omega-3 From Algae: What Actually Works?
Microalgae: The Real Omega-3 Sources
Provides DHA and EPA (directly usable forms)
Examples: Schizochytrium, Nannochloropsis
Used as algal oil supplements
Supports: Brain • Eyes • Heart • Anti-inflammatory
Common Edible Algae Or Seaweed: Spirulina / Chlorella / Nori: The Non Omega-3 Nutritional Supplements:
Negligible DHA and EPA
Provide: Protein • Minerals • Antioxidants • Iodine
Useful for general nutrition, but not for omega-3 needs
***
Practical Takeaway
Use microalgae-derived algal oil to obtain DHA and EPA
Include other algae for their general nutritional value, not for omega-3s
Do not rely solely on ALA sources for providing long-chain omega-3, DHA and EPA
***
Conclusion
Algae are very good sources of nutrition, but not all of them provide DHA and EPA. Microalgae-derived algal oil provides a direct, effective source of DHA and EPA, while other algae serve as supportive, nutrient-rich foods.
Related articles:
Large
The New Weight Loss Drugs — Science, Benefits And Misuse!
Benefits As Medical Treatment And Dangers Of Unethical, Casual Use!
A new class of medicines originally developed for diabetes has rapidly become the centre of a global weight loss craze.
Celebrities, influencers and social media personalities are discussing these injections as if they are shortcuts to an ideal body. Increasingly, even people who need to lose only a few kilograms are asking doctors whether they should start these medicines.
This trend needs careful scientific understanding.
***
What Are These Medicines?
The most commonly discussed drugs belong to a group called GLP-1 receptor agonists and related medicines.
Examples include:
Semaglutide
Tirzepatide
Liraglutide
Researchers are also developing newer and more powerful medicines including dual-agonist and triple-agonist drugs that act on multiple hormonal pathways related to appetite, metabolism and blood sugar control.
Some of the newer medicines attracting attention include:
Retatrutide
Orforglipron
CagriSema
Oral pill versions of some of these medicines are also becoming available, which may further increase their popularity and commercial use in the coming years.
While these newer drugs may improve weight loss in selected patients, they also raise concerns about increasing casual use, aggressive marketing and long-term overmedicalisation of body weight.
These medicines were originally developed for treating type 2 diabetes. Doctors later observed that many patients also lost weight while taking them.
***
How Do They Work?
These drugs mainly:
reduce appetite,
increase the feeling of fullness,
slow stomach emptying,
and improve blood sugar control.
Many patients naturally eat less while taking them.
***
Can They Help?
Yes — in properly selected overweight or obese individuals, especially those with:
diabetes,
prediabetes,
fatty liver disease,
metabolic syndrome,
abdominal obesity,
hypertension,
or sleep apnoea,
these medicines can sometimes produce meaningful weight reduction and metabolic improvement.
For severely obese individuals struggling despite sincere lifestyle changes, they may reduce long-term health risks.
***
The Growing Misuse
The problem is that these medicines are increasingly being used by:
mildly overweight people,
individuals wanting “camera-ready” appearances,
young adults influenced by social media,
and even normal-weight individuals afraid of gaining weight.
Medicines meant for obesity and metabolic disease are slowly being turned into cosmetic lifestyle products.
Weight Loss Alone Is Not Health
A person may lose weight and still become unhealthy.
Rapid weight loss without proper nutrition may reduce:
muscle mass,
strength,
stamina,
and nutritional reserves.
Especially in middle-aged and older individuals, excessive muscle loss can become a serious long-term problem.
The goal should not merely be ‘lighter weight’, but:
healthier metabolism,
lower abdominal fat,
improved strength,
better fitness,
and sustainable habits.
***
These Medicines Require Specialist Supervision
These are powerful prescription medicines and are usually best supervised by endocrinologists, diabetologists or cardiologists familiar with obesity-related metabolic disease.
Before starting treatment, doctors may need to assess:
blood sugar,
kidney and liver function,
pancreatic and gall bladder health,
cardiovascular risk,
nutritional status,
and existing medications.
Careful follow-up is important to monitor:
side effects,
hydration,
nutritional adequacy,
and muscle preservation.
***
Using these medicines casually for cosmetic slimming without proper supervision may expose otherwise healthy individuals to unnecessary risks.
Possible Side Effects
Common side effects include:
nausea,
vomiting,
acidity,
constipation,
diarrhoea,
bloating,
and fatigue.
More serious concerns may include:
gall bladder disease,
pancreatitis,
dehydration,
nutritional deficiencies,
and excessive muscle loss.
***
Another Important Reality — Weight Often Returns
Many people regain weight after stopping the medicine if lifestyle habits have not changed.
These medicines cannot permanently replace:
dietary discipline,
physical activity,
sleep regulation,
and behavioural change.
***
Final Message
These newer medicines represent an important scientific advance in obesity treatment and may genuinely help selected patients.
But their growing misuse reflects a larger commercial culture obsessed with appearance and rapid slimming.
Most of the use of these powerful prescription drugs in India is unethical, likely suggested by gym trainers and beauty clinics and word of mouth in social circles and parties, often procured from grey markets.
Such use is extremely dangerous.
Health should remain the primary goal — not simply becoming thinner for photographs, social approval or social media trends.
Related article
Which Algae Provide DHA And EPA?
Microalgae, Spirulina, Chlorella And Nori!
Why Most ‘Algae Superfoods” Don’t Meet Your Omega-3 Needs?
Most algae are promoted as nutritional superfoods—but not all of them provide the omega-3 fats your body actually needs. If you are relying on spirulina, chlorella, or seaweed for DHA and EPA, you may be missing a critical piece of the puzzle. This article explains which algae truly deliver these essential fats—and which do not.
Microalgae: The True Source Of DHA And EPA
DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) originate in marine microalgae—not in fish. Fish accumulate these fats by consuming algae, making microalgae the primary source in the food chain.
Certain species of microalgae are particularly rich in these long-chain omega-3s, DHA and EPA:
Schizochytrium – a concentrated source of DHA
Crypthecodinium cohnii – widely used for its DHA content
Nannochloropsis – a valuable source of EPA
These microalgae are cultivated and processed into algal oil, which forms the basis of most vegetarian and vegan omega-3 supplements. Unlike plant sources such as flaxseeds or walnuts, which provide ALA (alpha-linolenic acid), these deliver DHA and EPA directly—the forms the body actually uses.
This distinction matters because the conversion of ALA to DHA and EPA in humans is inefficient and often insufficient to meet physiological needs.
***
What Can You Actually Buy?
In practical terms, microalgae are not consumed directly as foods—they are available as algal oil supplements.
These typically come in:
Softgel capsules (most common)
Liquid algal oil (less common)
Most products provide DHA alone or a combination of DHA and EPA, usually in the range of 100–300 mg per serving. They are plant-based, fish-free, and sourced from controlled cultivation, making them a clean alternative to fish oil.
When choosing a supplement, the most useful label to check is the actual DHA and EPA content per serving, rather than just the term ‘omega-3’.
Other Algae: Nutritious, But Not Omega-3 Sources
Commonly consumed algae contribute valuable nutrients, but not meaningful amounts of DHA or EPA:
Spirulina – rich in protein and antioxidants like phycocyanin, but contains negligible DHA and EPA.
Chlorella – provides chlorophyll and micronutrients, without contributing significant DHA and EPA.
Nori (and other seaweeds) – a useful source of iodine, trace minerals, and fiber, but not a reliable source of DHA or EPA.
***
Why This Matters
Confusing these categories can create a false sense of nutritional adequacy. Regular intake of spirulina or seaweed does not ensure sufficient DHA and EPA.
For those who do not consume fatty fish, this gap is important, as DHA and EPA play key roles in brain function, vision, inflammation regulation, and cardiovascular health.
***
Quick Comparison: Microalgae Vs Common Edible Algae
Omega-3 From Algae: What Actually Works?
Microalgae: The Real Omega-3 Sources
Provides DHA and EPA (directly usable forms)
Examples: Schizochytrium, Nannochloropsis
Used as algal oil supplements
Supports: Brain • Eyes • Heart • Anti-inflammatory
Common Edible Algae Or Seaweed: Spirulina / Chlorella / Nori: The Non Omega-3 Nutritional Supplements:
Negligible DHA and EPA
Provide: Protein • Minerals • Antioxidants • Iodine
Useful for general nutrition, but not for omega-3 needs
***
Practical Takeaway
Use microalgae-derived algal oil to obtain DHA and EPA
Include other algae for their general nutritional value, not for omega-3s
Do not rely solely on ALA sources for providing long-chain omega-3, DHA and EPA
***
Conclusion
Algae are very good sources of nutrition, but not all of them provide DHA and EPA. Microalgae-derived algal oil provides a direct, effective source of DHA and EPA, while other algae serve as supportive, nutrient-rich foods.
Related articles:
Large Alt
The New Weight Loss Drugs — Science, Benefits And Misuse!
Benefits As Medical Treatment And Dangers Of Unethical, Casual Use!
A new class of medicines originally developed for diabetes has rapidly become the centre of a global weight loss craze.
Celebrities, influencers and social media personalities are discussing these injections as if they are shortcuts to an ideal body. Increasingly, even people who need to lose only a few kilograms are asking doctors whether they should start these medicines.
This trend needs careful scientific understanding.
***
What Are These Medicines?
The most commonly discussed drugs belong to a group called GLP-1 receptor agonists and related medicines.
Examples include:
Semaglutide
Tirzepatide
Liraglutide
Researchers are also developing newer and more powerful medicines including dual-agonist and triple-agonist drugs that act on multiple hormonal pathways related to appetite, metabolism and blood sugar control.
Some of the newer medicines attracting attention include:
Retatrutide
Orforglipron
CagriSema
Oral pill versions of some of these medicines are also becoming available, which may further increase their popularity and commercial use in the coming years.
While these newer drugs may improve weight loss in selected patients, they also raise concerns about increasing casual use, aggressive marketing and long-term overmedicalisation of body weight.
These medicines were originally developed for treating type 2 diabetes. Doctors later observed that many patients also lost weight while taking them.
***
How Do They Work?
These drugs mainly:
reduce appetite,
increase the feeling of fullness,
slow stomach emptying,
and improve blood sugar control.
Many patients naturally eat less while taking them.
***
Can They Help?
Yes — in properly selected overweight or obese individuals, especially those with:
diabetes,
prediabetes,
fatty liver disease,
metabolic syndrome,
abdominal obesity,
hypertension,
or sleep apnoea,
these medicines can sometimes produce meaningful weight reduction and metabolic improvement.
For severely obese individuals struggling despite sincere lifestyle changes, they may reduce long-term health risks.
***
The Growing Misuse
The problem is that these medicines are increasingly being used by:
mildly overweight people,
individuals wanting “camera-ready” appearances,
young adults influenced by social media,
and even normal-weight individuals afraid of gaining weight.
Medicines meant for obesity and metabolic disease are slowly being turned into cosmetic lifestyle products.
Weight Loss Alone Is Not Health
A person may lose weight and still become unhealthy.
Rapid weight loss without proper nutrition may reduce:
muscle mass,
strength,
stamina,
and nutritional reserves.
Especially in middle-aged and older individuals, excessive muscle loss can become a serious long-term problem.
The goal should not merely be ‘lighter weight’, but:
healthier metabolism,
lower abdominal fat,
improved strength,
better fitness,
and sustainable habits.
***
These Medicines Require Specialist Supervision
These are powerful prescription medicines and are usually best supervised by endocrinologists, diabetologists or cardiologists familiar with obesity-related metabolic disease.
Before starting treatment, doctors may need to assess:
blood sugar,
kidney and liver function,
pancreatic and gall bladder health,
cardiovascular risk,
nutritional status,
and existing medications.
Careful follow-up is important to monitor:
side effects,
hydration,
nutritional adequacy,
and muscle preservation.
***
Using these medicines casually for cosmetic slimming without proper supervision may expose otherwise healthy individuals to unnecessary risks.
Possible Side Effects
Common side effects include:
nausea,
vomiting,
acidity,
constipation,
diarrhoea,
bloating,
and fatigue.
More serious concerns may include:
gall bladder disease,
pancreatitis,
dehydration,
nutritional deficiencies,
and excessive muscle loss.
***
Another Important Reality — Weight Often Returns
Many people regain weight after stopping the medicine if lifestyle habits have not changed.
These medicines cannot permanently replace:
dietary discipline,
physical activity,
sleep regulation,
and behavioural change.
***
Final Message
These newer medicines represent an important scientific advance in obesity treatment and may genuinely help selected patients.
But their growing misuse reflects a larger commercial culture obsessed with appearance and rapid slimming.
Most of the use of these powerful prescription drugs in India is unethical, likely suggested by gym trainers and beauty clinics and word of mouth in social circles and parties, often procured from grey markets.
Such use is extremely dangerous.
Health should remain the primary goal — not simply becoming thinner for photographs, social approval or social media trends.
Related article
Which Algae Provide DHA And EPA?
Microalgae, Spirulina, Chlorella And Nori!
Why Most ‘Algae Superfoods” Don’t Meet Your Omega-3 Needs?
Most algae are promoted as nutritional superfoods—but not all of them provide the omega-3 fats your body actually needs. If you are relying on spirulina, chlorella, or seaweed for DHA and EPA, you may be missing a critical piece of the puzzle. This article explains which algae truly deliver these essential fats—and which do not.
Microalgae: The True Source Of DHA And EPA
DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid) originate in marine microalgae—not in fish. Fish accumulate these fats by consuming algae, making microalgae the primary source in the food chain.
Certain species of microalgae are particularly rich in these long-chain omega-3s, DHA and EPA:
Schizochytrium – a concentrated source of DHA
Crypthecodinium cohnii – widely used for its DHA content
Nannochloropsis – a valuable source of EPA
These microalgae are cultivated and processed into algal oil, which forms the basis of most vegetarian and vegan omega-3 supplements. Unlike plant sources such as flaxseeds or walnuts, which provide ALA (alpha-linolenic acid), these deliver DHA and EPA directly—the forms the body actually uses.
This distinction matters because the conversion of ALA to DHA and EPA in humans is inefficient and often insufficient to meet physiological needs.
***
What Can You Actually Buy?
In practical terms, microalgae are not consumed directly as foods—they are available as algal oil supplements.
These typically come in:
Softgel capsules (most common)
Liquid algal oil (less common)
Most products provide DHA alone or a combination of DHA and EPA, usually in the range of 100–300 mg per serving. They are plant-based, fish-free, and sourced from controlled cultivation, making them a clean alternative to fish oil.
When choosing a supplement, the most useful label to check is the actual DHA and EPA content per serving, rather than just the term ‘omega-3’.
Other Algae: Nutritious, But Not Omega-3 Sources
Commonly consumed algae contribute valuable nutrients, but not meaningful amounts of DHA or EPA:
Spirulina – rich in protein and antioxidants like phycocyanin, but contains negligible DHA and EPA.
Chlorella – provides chlorophyll and micronutrients, without contributing significant DHA and EPA.
Nori (and other seaweeds) – a useful source of iodine, trace minerals, and fiber, but not a reliable source of DHA or EPA.
***
Why This Matters
Confusing these categories can create a false sense of nutritional adequacy. Regular intake of spirulina or seaweed does not ensure sufficient DHA and EPA.
For those who do not consume fatty fish, this gap is important, as DHA and EPA play key roles in brain function, vision, inflammation regulation, and cardiovascular health.
***
Quick Comparison: Microalgae Vs Common Edible Algae
Omega-3 From Algae: What Actually Works?
Microalgae: The Real Omega-3 Sources
Provides DHA and EPA (directly usable forms)
Examples: Schizochytrium, Nannochloropsis
Used as algal oil supplements
Supports: Brain • Eyes • Heart • Anti-inflammatory
Common Edible Algae Or Seaweed: Spirulina / Chlorella / Nori: The Non Omega-3 Nutritional Supplements:
Negligible DHA and EPA
Provide: Protein • Minerals • Antioxidants • Iodine
Useful for general nutrition, but not for omega-3 needs
***
Practical Takeaway
Use microalgae-derived algal oil to obtain DHA and EPA
Include other algae for their general nutritional value, not for omega-3s
Do not rely solely on ALA sources for providing long-chain omega-3, DHA and EPA
***
Conclusion
Algae are very good sources of nutrition, but not all of them provide DHA and EPA. Microalgae-derived algal oil provides a direct, effective source of DHA and EPA, while other algae serve as supportive, nutrient-rich foods.
Related articles: