The Relationship Between Visceral Fat And PCOS Or PMOS!
The Hidden Hormonal Connection Between Visceral Fat, Hyperinsulinemia And PCOS Or PMOS!
Many young women today are troubled by a combination of symptoms that often seem unrelated at first glance.
Their menstrual cycles become irregular. They begin to gain weight, particularly around the abdomen. Acne persists beyond adolescence. Some develop excessive facial hair, while others later encounter difficulty in conceiving.
In a large number of such cases, the underlying condition turns out to be Polycystic Ovary Syndrome (PCOS).
For many years PCOS was thought of mainly as a disorder of the ovaries. Modern research has revealed a far more complex picture. PCOS is now recognised as a condition that involves not only the reproductive organs but also the metabolic and hormonal systems of the body.
At the centre of this process lies a powerful but often overlooked factor — excess abdominal fat and the hormonal disturbance known as hyperinsulinemia.
***
PCOS Is Now Increasingly Being Called PMOS
An important recent development is that international experts have begun replacing the term PCOS with PMOS — Polyendocrine Metabolic Ovarian Syndrome.
The newer name reflects modern scientific understanding more accurately. Many women with the condition do not actually have ovarian cysts, while the disorder affects not only the ovaries, but also metabolism, insulin regulation, hormones, body fat distribution, emotional disturbances, skin, fertility and long-term cardiovascular health.
Many people are also familiar with the older term PCOD (Polycystic Ovarian Disease). Modern medical understanding now recognises that PCOD and PCOS largely refer to the same condition, with PCOS — and increasingly PMOS — being the preferred terminology.
Most importantly, PMOS is not merely an ovarian disorder. It is a complex condition involving the body’s metabolic and hormonal systems.
***
The Special Role of Visceral Fat
Not all body fat behaves in the same way.
The fat that lies just beneath the skin is called subcutaneous fat. In contrast, visceral fat accumulates deep within the abdomen around vital organs such as the liver, pancreas and intestines.
This fat is far more metabolically active. Instead of simply storing energy, visceral fat releases a variety of substances that influence metabolism and hormone regulation.
As visceral fat increases, the body’s sensitivity to insulin gradually declines. This condition is known as insulin resistance.
When Insulin Levels Rise
Insulin is the hormone that allows glucose in the blood to enter the body’s cells to produce energy.
When cells become resistant to insulin, the pancreas tries to compensate by producing larger amounts of insulin. This results in chronically elevated insulin levels, a condition called hyperinsulinemia.
For a long time, insulin was viewed mainly as a hormone involved in blood sugar control. We now know that insulin also has powerful effects on many other organs, including the ovaries.
How High Insulin Affects the Ovaries
High insulin levels can stimulate the ovaries to produce excess male hormones known as androgens.
These hormonal changes interfere with the normal process of ovulation. Instead of one follicle maturing and releasing an egg each month, multiple small follicles may begin to develop but fail to mature properly.
This leads to the characteristic appearance of polycystic ovaries and contributes to the symptoms commonly associated with PCOS.
These may include:
irregular or infrequent menstrual periods
acne and oily skin
excess facial or body hair
thinning of scalp hair
difficulty in conceiving
Thus, the hormonal disturbance seen in PCOS is often closely linked to insulin resistance and hyperinsulinemia.
***
The Vicious Cycle
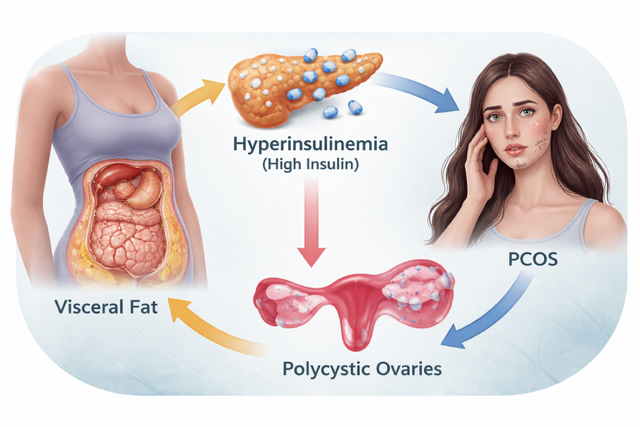
One of the most challenging aspects of PCOS or PMOS is the cycle that can develop between abdominal fat, insulin resistance and hormonal imbalance.
Excess visceral fat promotes insulin resistance. Insulin resistance leads to higher insulin levels. Elevated insulin stimulates the ovaries to produce more androgens. These hormonal changes can further promote abdominal fat accumulation.
The cycle can therefore reinforce itself:
Visceral fat → insulin resistance → hyperinsulinemia → excess androgens → worsening PCOS.
Breaking this cycle is often the key to improving the condition.
PCOS or PMOS and Long-Term Metabolic Health
Because insulin resistance plays such a central role, PCOS or PMOS is now recognised not only as a reproductive disorder but also as a metabolic condition.
Women with PMOS have a higher risk of developing conditions such as:
Type 2 Diabetes
Metabolic Syndrome
Nonalcoholic Fatty Liver Disease
These risks are closely related to the presence of insulin resistance and abdominal obesity.
The Encouraging News
Despite these concerns, there is also encouraging news.
Even modest improvements in lifestyle can significantly improve insulin sensitivity and reduce the hormonal imbalance associated with PCOS.
Weight reduction, particularly the loss of abdominal fat, can help lower insulin levels and restore more normal hormonal patterns.
Regular physical activity improves the body’s response to insulin, while balanced nutrition helps prevent large spikes in insulin levels after meals.
Studies have shown that even a 5–10 percent reduction in body weight can lead to meaningful improvements in menstrual regularity and fertility in many women with PMOS.
Understanding the Underlying Mechanism
Recognising the role of visceral fat and hyperinsulinemia helps us understand why PCOS has become more common in recent decades.
Changes in lifestyle, reduced physical activity and increased consumption of highly refined foods can all contribute to the development of abdominal obesity and insulin resistance.
Addressing these factors early can therefore play an important role in preventing or controlling the condition.
A Final Thought:
PCOS or PMOS has become one of the most common hormonal disorders affecting young women today. Yet it is also a condition in which knowledge and early action can make a profound difference.
By understanding the connection between visceral fat, insulin resistance and hormonal balance, many women can take steps that not only improve their reproductive health but also protect their long-term metabolic wellbeing.
Related articles:
‘Health Problems Of The Young: PCOS!’
‘Overcoming PCOS And Infertility: The Role Of Weight Loss in Fertility Treatment!’